
Executive Summary
Veterans in the United States continue to face a silent crisis in the form of suicide, mental health challenges, and underutilization of earned benefits. In 2023, 6,398 veterans died by suicide—an average of 17.5 deaths per day—despite decades of investment in prevention and support programming. At the same time, roughly 15.8 million veterans represent 6.1% of the U.S. adult population, making this a national-scale public health and moral imperative.
This white paper argues that VA Disability Benefits are structurally aligned with Maslow’s Hierarchy of Needs, providing a pathway from basic survival to self-actualization for veterans transitioning into civilian life. When effectively accessed, these benefits support:
- Physiological needs through income, housing stability, and healthcare access
- Safety needs through long-term financial security and ongoing medical treatment
- Love and belonging through access to VA care, peer support, and community programs
- Esteem through formal recognition of service-connected injuries and opportunities for education and employment
- Self-actualization through the freedom and resources to pursue purpose, growth, and meaningful post-service careers
However, over 30% of veterans who may be eligible never file for VA Disability Benefits, often due to confusion, complexity, stigma, or misinformation. Simultaneously, VA data show that more than 60% of veterans who die by suicide were not engaged in VA health care in the year before their death, underscoring the consequences of under-enrollment and disengagement from the system.
In 2026, the VA is implementing significant reforms to its mental health rating criteria, including eliminating the 0% rating and establishing a minimum 10% rating for any service-connected mental health condition. These changes are expected to expand access to compensation, reduce rating ambiguity, and more accurately reflect the real-world impact of mental health conditions on veterans’ lives.
VetsForever exists to ensure that no veteran has to navigate this system alone. By combining claims expertise, legal guidance, and trauma-informed support, VetsForever helps veterans secure the benefits they have earned—benefits that are not merely financial transactions, but foundational building blocks of healing, dignity, and long-term well-being.
1. The Ongoing Crisis for Veterans
1.1 Scope of the Challenge
The data tell a sobering story:
- In 2023, there were 6,398 veteran suicides in the United States, down slightly from 6,442 in 2022, translating to an average of 17.5 veteran suicides per day.
- The suicide rate among veterans rose to 35.2 per 100,000 in 2023, the highest rate since at least 2018.
- Approximately 15.8 million veterans lived in the U.S. in 2023, representing 6.1% of the civilian population aged 18 and older.
- Despite small numerical improvements in total suicides, the rate per capita has increased, and more than 140,000 veterans have died by suicide since 2001, leading advocacy groups to describe the situation as remaining at “epidemic levels.”
1.2 Suicide Trends, 2022–2023
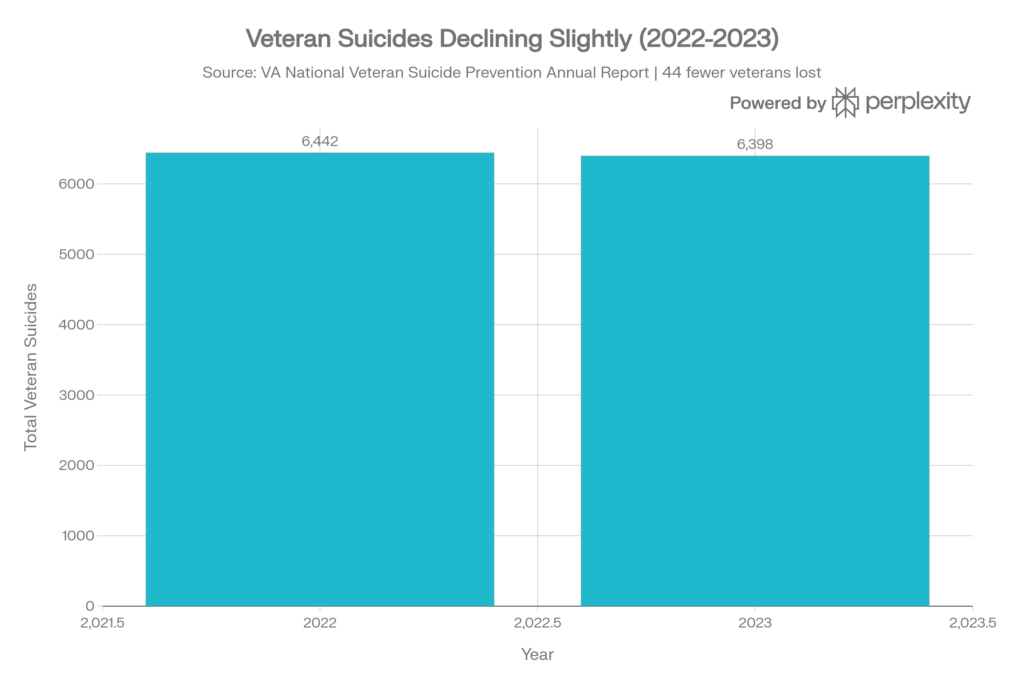
While total veteran suicides and the daily suicide average decreased slightly between 2022 and 2023, the change is marginal and insufficient to be considered a substantive improvement.
Critically, VA data show that roughly 61% of veterans who died by suicide in 2023 were not receiving VA health care in the last year of their lives, underlining a significant engagement gap. This disconnect reveals that outreach, education on benefits, and navigation support are as crucial as the existence of programs themselves.
2. Transition, Mental Health, and Barriers to Care
The first year after separation from military service is often the most destabilizing for veterans—characterized by the loss of structure, camaraderie, and mission, which can amplify underlying mental health conditions such as PTSD, depression, anxiety, and substance use disorders.
Research indicates that many veterans do not seek mental health treatment, and fewer than half of those who could benefit from services receive consistent care. Early engagement in care and benefits within the first year of separation is associated with better long-term mental health outcomes and reduced suicidality.
Yet, more than 30% of veterans who may be eligible for VA Disability Benefits never file a claim, leaving substantial financial, medical, and psychosocial support on the table.
Common barriers include:
- Confusion over eligibility and what conditions can be claimed
- Overwhelming paperwork and complex evidence requirements
- Long wait times for decisions and appeals
- Stigma and fear of being perceived as “weak” or “less capable” by employers or peers
- Misunderstanding of the differences between VA Disability Benefits and Social Security Disability programs (SSDI/SSI)
These barriers do not just delay payments—they delay stabilization at the very base of Maslow’s hierarchy, preventing veterans from building toward higher levels of recovery and purpose.
3. Maslow’s Hierarchy of Needs and VA Disability Benefits
Maslow’s Hierarchy of Needs describes a progression of human motivation from basic survival to the realization of full potential. When viewed through a veteran-centered lens, VA Disability Benefits can be seen as a structured mechanism to meet these layered needs.
3.1 Physiological Needs: Survival and Health
Physiological needs include food, shelter, rest, and medical care. For many veterans, disability compensation is a critical protective factor against homelessness, food insecurity, and untreated chronic health conditions.
Even a 10% disability rating provides monthly tax-free income that can cover basic expenses or co-pays, while higher ratings increasingly offset the costs of housing, utilities, and health care. When physiological needs are met through predictable benefits and healthcare access, veterans can redirect energy away from survival anxiety and toward engagement in treatment, work, family life, and education.
3.2 Safety Needs: Financial and Emotional Security
Safety needs encompass personal security, health security, and financial stability. For veterans, this often means:
- A dependable monthly income from disability benefits
- Access to VA health care and mental health services
- Legal protections and assistance with claims and appeals
The VA’s own reporting emphasizes that veterans engaged with VA health care and benefits have stronger protective factors against suicide. Disability benefits help reduce acute financial crises—such as evictions, utility shut-offs, and medical debt—that are known stressors and potential triggers for mental health deterioration.
Under 2026 mental health rating criteria, disability ratings will be more tightly linked to functional impairment and symptom severity, independent of employment status, making the safety net more responsive to real-world risk.
3.3 Love and Belonging: Community and Connection
Maslow’s third level highlights the importance of relationships and acceptance. Many veterans describe feeling profoundly “alone in a crowd” after separation, especially when managing invisible wounds like PTSD or moral injury.
Disability benefits promote belonging in several ways:
- They connect veterans to VA facilities where they can access group therapy, peer support, and veteran-specific programs.
- Participation in veterans’ organizations, support groups, and nonprofit programs is often facilitated by having both the time and resources enabled by disability compensation.
- Research shows that social isolation is a powerful predictor of suicidal ideation, and that meaningful connection—through family, peers, and community—significantly improves mental health outcomes.
3.4 Esteem Needs: Recognition, Dignity, and Opportunity
Esteem needs involve respect, self-respect, recognition, and a sense of contribution. For many veterans, the disability rating decision itself carries deep symbolic weight: it is the institution’s acknowledgment that their injuries and sacrifices are real and consequential.
Voices from veteran advocacy communities consistently note that receiving a disability rating often enhances veterans’ sense of legitimacy and reduces self-blame. Disability compensation also enables education and job retraining, which can improve self-efficacy and perceived employability, further bolstering self-esteem.
3.5 Self-Actualization: Purpose Beyond Service
Self-actualization is the realization of one’s full potential. For veterans, this may mean:
- Completing a degree or professional certification
- Launching a business or nonprofit
- Serving as mentors, advocates, or community leaders
- Pursuing creative, spiritual, or family-centered goals
VA education and rehabilitation programs—such as Veteran Readiness and Employment (VR&E) and GI Bill–linked opportunities—are easier to pursue when disability benefits have stabilized a veteran’s basic and safety needs. Under the 2026 mental health rating changes, veterans with significant psychological injuries will be more likely to receive compensation commensurate with their functional limitations, allowing them to allocate time and resources toward growth, rather than mere survival.
4. 2026 VA Mental Health Rating Reforms
The VA is modernizing the Schedule for Rating Disabilities, including the mental health section, with changes expected to take effect in 2026. Key features include:
- Elimination of the 0% rating for mental health: All service-connected mental health conditions will receive at least a 10% rating, ensuring that every recognized condition results in compensation.
- Minimum 10% rating for any diagnosed service-connected mental health condition: This acknowledges that even mild conditions can carry functional impact and require ongoing management.
- Domain-based functional evaluation: Ratings will consider levels of impairment across multiple life domains (work, social relationships, self-care) rather than relying solely on vague descriptions of “mild,” “moderate,” or “severe” impairment.
- More direct linkage between symptom severity and higher ratings: Veterans may qualify for 70% or 100% ratings based on functional limitations and symptom frequency, even if they remain employed.
These reforms are intended to reduce ambiguity in mental health ratings, better reflect contemporary clinical understanding of psychological injuries, ensure fairer and more consistent compensation, and encourage more veterans to come forward with mental health claims.
By design, these changes reinforce Maslow’s framework: they strengthen the financial and clinical foundation that allows veterans to move up the pyramid toward belonging, esteem, and self-actualization.
5. Why Veterans Don’t Apply—and What Must Change
Despite the clear alignment between disability benefits and veterans’ core needs, many veterans never access the system or disengage partway through. Common reasons include:
- Confusion and misinformation about eligibility, secondary conditions, and filing multiple claims
- Administrative burden: assembling medical evidence, service records, and detailed statements is time-consuming and overwhelming
- Discouragement after initial denials or low ratings, leading to abandonment of claims
- Employment concerns: fear that being “labeled disabled” will damage career prospects or lead colleagues to view them differently
- Conflation with Social Security Disability: misunderstandings about income limits, work requirements, and the distinct nature of VA Disability Benefits
Each of these barriers undermines progress at the lower tiers of Maslow’s hierarchy, prolonging financial insecurity and delaying access to mental health care, peer networks, and growth opportunities.
6. The Role of VetsForever
VetsForever exists to bridge the gap between eligibility and access—between theory and lived reality. As an organization, VetsForever:
- Provides step-by-step guidance through the VA claims process, from initial filing to appeals
- Offers education on what conditions can be claimed, how to document them, and how to avoid common pitfalls
- Partners with legal and medical professionals to strengthen evidence for claims, including mental health claims under the new 2026 criteria
- Emphasizes trauma-informed engagement, recognizing that paperwork, evaluations, and hearings can be triggering for veterans with PTSD or anxiety
- Connects veterans to community resources, including mental health providers, peer support groups, and employment and education programs
By doing so, VetsForever helps veterans shore up the foundation of Maslow’s hierarchy—physiological and safety needs—so they can rebuild belonging, esteem, and self-actualization on solid ground.
7. From Survival to Self-Actualization: A Call to Action
VA Disability Benefits are not charity; they are earned instruments of justice and restoration. When properly understood and accessed, they:
- Reduce financial distress and homelessness
- Improve access and adherence to mental health treatment
- Strengthen social connection and family stability
- Affirm dignity, service, and sacrifice
- Enable long-term growth, education, and purpose
The data are clear: most veterans who die by suicide were not connected to VA care, and many others never file claims despite eligibility. Closing this gap requires coordinated action from government, nonprofits, employers, and communities—supported by mission-driven organizations like VetsForever.
VetsForever is committed to a future in which every veteran:
- Understands the benefits they have earned
- Has expert guidance to navigate the VA system
- Receives timely, fair, and adequate compensation
- Is empowered to move beyond survival toward a fulfilling, purpose-driven life
When we align policy, practice, and support with Maslow’s Hierarchy of Needs, we do more than administer a benefits system—we create a continuum of care that honors service, protects life, and unlocks human potential.
Sources
- Military.com – VA Releases Newest Veteran Suicide Data
- VA News – Annual Veteran Suicide Prevention Report (2023 Data)
- Door County Pulse – Honoring Veterans Day 2024
- The National Desk – Stopping Veteran Suicide: VA Face the Fight
- U.S. Census Bureau – Veterans Day Facts for Features 2024
- YouTube – VA Mental Health Rating Reforms (Video)
- VA Data – VetPop2023 Data Story
- WEAR TV – VA’s 2025 Report on Veteran Suicide




